Health
Understanding Heterotopic Pregnancy: Causes, Symptoms, and Treatment
Introduction
Pregnancy is usually a joyful time, but in rare cases, it can take an unexpected and dangerous turn. One such condition is heterotopic pregnancy when two pregnancies occur simultaneously, one inside the uterus (normal) and the other outside, typically in the fallopian tube. Although rare, this condition can be life-threatening if not recognized and treated promptly.
Understanding Normal Pregnancy
In a healthy pregnancy, a fertilized egg travels through the fallopian tube to the uterus, where it implants in the uterine lining. The uterus provides the perfect environment for the embryo to grow and develop. However, in some cases, the fertilized egg doesn’t make it to the uterus and implants elsewhere, leading to an ectopic pregnancy. In heterotopic pregnancy, both occur together one normal, one abnormal.
What Happens in Heterotopic Pregnancy
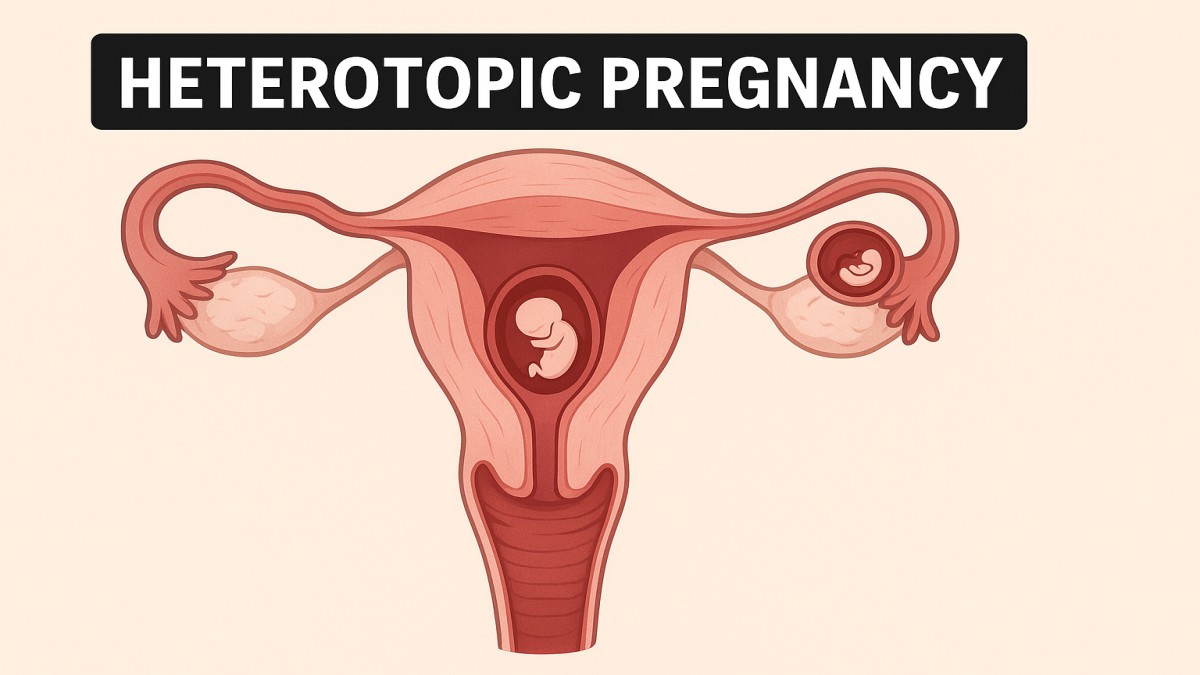
A heterotopic pregnancy involves two simultaneous implantations:
- One intrauterine (in the uterus).
- One ectopic, often in the fallopian tube, ovary, or abdominal cavity.
This dual implantation makes diagnosis difficult, as doctors might focus on the healthy intrauterine pregnancy, missing the hidden danger of the ectopic one.
Prevalence and Risk Factors
In natural conception, heterotopic pregnancy is extremely rare occurring in 1 out of 30,000 pregnancies. However, with the rise of assisted reproductive technologies (ART) like IVF, the incidence has increased to as high as 1 in 100 pregnancies in some cases.
Major Risk Factors Include:
- Fertility treatments (IVF, IUI)
- Pelvic inflammatory disease (PID)
- Tubal surgery or damage
- Previous ectopic pregnancy
- Endometriosis
Causes of Heterotopic Pregnancy
The condition can arise due to several biological and medical factors:
1. Assisted Reproductive Technologies (ART)
During IVF, multiple embryos may be transferred to increase chances of conception, which can result in dual implantation.
2. Tubal Damage
Inflammation or scarring in the fallopian tubes can hinder the movement of a fertilized egg, leading to ectopic implantation.
3. Hormonal or Structural Abnormalities
Hormonal imbalances or unusual uterine structures can influence implantation locations.
Symptoms of Heterotopic Pregnancy
The symptoms often mimic normal pregnancy or other abdominal issues, making diagnosis challenging. Common signs include:
- Abdominal or pelvic pain
- Vaginal bleeding
- Shoulder tip pain (due to internal bleeding)
- Dizziness or fainting
- Enlarged uterus (due to intrauterine pregnancy)
If the ectopic component ruptures, it can cause severe internal bleeding, a medical emergency requiring immediate attention.
How It Is Diagnosed
Diagnosing heterotopic pregnancy is complex because the presence of a normal intrauterine pregnancy can mask the ectopic one.
1. Ultrasound Imaging
A transvaginal ultrasound can reveal both pregnancies — one in the uterus and one outside it.
2. Blood Tests
Levels of β-hCG hormone can confirm pregnancy but may not distinguish between normal and ectopic pregnancies.
3. Laparoscopy
In unclear cases, laparoscopy (a minimally invasive surgery) may be performed for direct visualization and confirmation.
Challenges in Diagnosis
Because the symptoms overlap with those of a normal pregnancy, heterotopic pregnancy often goes unnoticed until complications arise. Even experienced clinicians can miss it if they rely solely on the presence of an intrauterine pregnancy.
Complications of Heterotopic Pregnancy
The most serious complication is rupture of the ectopic pregnancy, leading to internal bleeding, hypovolemic shock, and even death if untreated. Additionally, the treatment must be handled carefully to avoid harming the intrauterine fetus.
Treatment Options
1. Surgical Treatment
Laparoscopic surgery is the preferred treatment, as it allows removal of the ectopic pregnancy while preserving the intrauterine one.
2. Medical Management
Common drugs like methotrexate used for ectopic pregnancies are not suitable in heterotopic cases since they can harm the viable uterine pregnancy.
Conclusion
Heterotopic pregnancy, though rare, is a serious medical condition that demands awareness, timely diagnosis, and expert care. With advancements in imaging and surgical techniques, it’s possible to manage this complex condition successfully, preserving both the mother’s health and, in many cases, the intrauterine pregnancy.
FAQs
1. Can heterotopic pregnancy occur naturally without IVF?
Yes, although very rare, it can occur naturally, especially in women with tubal damage or prior ectopic pregnancies.
2. How soon can heterotopic pregnancy be detected?
Usually between 5–8 weeks of gestation through ultrasound and clinical symptoms.
3. Can the intrauterine baby survive after surgery?
Yes, if the ectopic part is treated carefully, many women go on to have healthy full-term babies.
4. What is the recurrence risk of heterotopic pregnancy?
While recurrence is rare, women with previous ectopic pregnancies or tubal damage have a slightly higher risk.
5. What should I do if I experience sharp pain during early pregnancy?
Seek immediate medical care. Even mild pain during pregnancy can signal serious conditions like ectopic or heterotopic pregnancy.

 entertainment8 months ago
entertainment8 months agoPYT Telegram: A Complete Guide to Understanding, Using, and Maximizing It

 entertainment9 months ago
entertainment9 months agoOnionFlix: Everything You Need to Know About This Streaming Website

 others7 months ago
others7 months agoNook vs Kindle: Which E-Reader Is Right for You?

 gaming9 months ago
gaming9 months agoMelisandre: The Enigmatic Priestess of Game of Thrones

























